Items filtered by date: November 2023
Who Is at Risk for Ingrown Toenails?
 Ingrown toenails occur when the edge of a toenail grows into the surrounding skin, causing pain, swelling, and sometimes infection. Those at higher risk include individuals with curved or thick nails, those who trim their nails improperly, people who wear tight or ill-fitting shoes, and athletes or dancers who frequently stress their feet. Symptoms of ingrown toenails include redness, swelling, pain along the nail edges, and, in severe cases, pus or infection. Common causes are improper nail trimming, trauma to the toenail, and genetic predisposition. To prevent ingrown toenails, trim nails straight across, avoid cutting them too short, and wear shoes that provide adequate space for the toes. Relief for mild cases includes soaking the foot in warm water and keeping the foot clean. If you have severe symptoms of an ingrown toenail or it appears infected, it is strongly suggested that you schedule an appointment with a podiatrist who may prescribe antibiotics or possibly a minor surgical procedure.
Ingrown toenails occur when the edge of a toenail grows into the surrounding skin, causing pain, swelling, and sometimes infection. Those at higher risk include individuals with curved or thick nails, those who trim their nails improperly, people who wear tight or ill-fitting shoes, and athletes or dancers who frequently stress their feet. Symptoms of ingrown toenails include redness, swelling, pain along the nail edges, and, in severe cases, pus or infection. Common causes are improper nail trimming, trauma to the toenail, and genetic predisposition. To prevent ingrown toenails, trim nails straight across, avoid cutting them too short, and wear shoes that provide adequate space for the toes. Relief for mild cases includes soaking the foot in warm water and keeping the foot clean. If you have severe symptoms of an ingrown toenail or it appears infected, it is strongly suggested that you schedule an appointment with a podiatrist who may prescribe antibiotics or possibly a minor surgical procedure.
Ingrown toenails can become painful if they are not treated properly. For more information about ingrown toenails, contact Thomas Vail, DPM of Step Alive Foot & Ankle Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
Ingrown Toenails
Ingrown toenails occur when a toenail grows sideways into the bed of the nail, causing pain, swelling, and possibly infection.
Causes
- Bacterial infections
- Improper nail cutting such as cutting it too short or not straight across
- Trauma to the toe, such as stubbing, which causes the nail to grow back irregularly
- Ill-fitting shoes that bunch the toes too close together
- Genetic predisposition
Prevention
Because ingrown toenails are not something found outside of shoe-wearing cultures, going barefoot as often as possible will decrease the likeliness of developing ingrown toenails. Wearing proper fitting shoes and using proper cutting techniques will also help decrease your risk of developing ingrown toenails.
Treatment
Ingrown toenails are a very treatable foot condition. In minor cases, soaking the affected area in salt or antibacterial soaps will not only help with the ingrown nail itself, but also help prevent any infections from occurring. In more severe cases, surgery is an option. In either case, speaking to your podiatrist about this condition will help you get a better understanding of specific treatment options that are right for you.
If you have any questions please feel free to contact our office located in Findlay, OH . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Various Causes of Ankle Pain
Ankles are joints that connect bones in the feet with bones in the lower leg. They are comprised of bones, ligaments, muscles, tendons, blood vessels, and nerves. The ankle joint allows the foot to move side-to-side, as well as up-and-down.
Ankle pain can be caused by a variety of conditions, but is most commonly due to soft tissue injuries such as ankle sprains and strains.
An ankle sprain occurs when one or more of the strong ligaments that support and stabilize the ankle become overly stretched or even torn if the ankle rolls, turns, or twists awkwardly. Depending on the grade of sprain (mild-moderate-severe), there will be varying degrees of pain, swelling, and restricted range of motion, along with tenderness, bruising, and ankle instability. There may even be an audible popping noise at the moment of injury.
Ankle strains can sometimes produce similar symptoms of pain, swelling, and loss of motion, however, they are due to overly stretched muscles and tendons—not ligaments. Ankle strains may also cause muscle cramps in the feet, calves and shins.
Ankle fractures are another common source of ankle pain and occur one or more of the three bones in the ankle become fractured (broken). These breaks can be stress fractures (due to repetitive stress) or traumatic fractures (due to an acute injury). Depending on where and how severe the fracture is, symptoms can include pain and swelling that can sometimes spread up to the knee, bruising or discoloration, and an inability to bear weight. A visible deformity or exposed bone may occur in severe fractures.
Various forms of arthritis may also cause ankle pain. Rheumatoid arthritis (RA) causes the immune system to attack healthy joints, like the ankle joint, by mistake, causing stiffness and swelling in both ankles. Osteoarthritis occurs when cartilage covering the ends of bones wears down, causing the bones to rub against each other. This results in pain, stiffness, and reduced range of motion in the ankle. Gout is a form of arthritis where excess amounts of uric acid in the bloodstream crystallize and build up on joints, causing severe pain and swelling. Reactive arthritis causes joint pain and swelling in the ankle in response to an infection in another part of the body.
Other forms of ankle pain include bursitis (an inflammation of a cushioning bursa sac between tendons and bone), scleroderma (a thickening of connective tissues), chronic ankle instability (caused by improperly healed ankle sprains), Achilles tendon injuries, flat feet, or an infection in the ankle.
Ankle Pain Caused by Arthritis
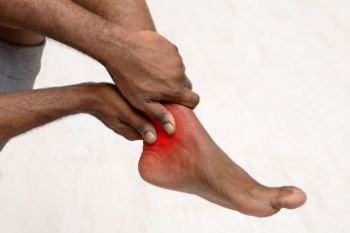 Ankle pain from arthritis can impact your daily life substantially. Ankle arthritis occurs when the joints in your ankles become inflamed. This can lead to pain, stiffness, and restricted movement. The three types of arthritis that can affect the ankles are osteoarthritis, rheumatoid arthritis, and gout. Osteoarthritis is caused by the gradual wearing away of cartilage in the joints, causing the bones to rub against other bones. Rheumatoid arthritis is a type of arthritis where the body's immune system attacks the joints by mistake and causes inflammation. Gout is a type of arthritis that causes pain, redness, and tenderness in your joints for a week or two, then returns to normal. No matter what the type is, ankle arthritis can make daily activities like walking or standing painful and challenging. If you are experiencing ankle pain, especially in the joints, it is suggested that you consult a podiatrist, or foot doctor, to find the best treatment options.
Ankle pain from arthritis can impact your daily life substantially. Ankle arthritis occurs when the joints in your ankles become inflamed. This can lead to pain, stiffness, and restricted movement. The three types of arthritis that can affect the ankles are osteoarthritis, rheumatoid arthritis, and gout. Osteoarthritis is caused by the gradual wearing away of cartilage in the joints, causing the bones to rub against other bones. Rheumatoid arthritis is a type of arthritis where the body's immune system attacks the joints by mistake and causes inflammation. Gout is a type of arthritis that causes pain, redness, and tenderness in your joints for a week or two, then returns to normal. No matter what the type is, ankle arthritis can make daily activities like walking or standing painful and challenging. If you are experiencing ankle pain, especially in the joints, it is suggested that you consult a podiatrist, or foot doctor, to find the best treatment options.
Ankle pain can have many different causes and the pain may potentially be serious. If you have ankle pain, consult with Thomas Vail, DPM from Step Alive Foot & Ankle Center. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Ankle pain is any condition that causes pain in the ankle. Due to the fact that the ankle consists of tendons, muscles, bones, and ligaments, ankle pain can come from a number of different conditions.
Causes
The most common causes of ankle pain include:
- Types of arthritis (rheumatoid, osteoarthritis, and gout)
- Ankle sprains
- Broken ankles
- Achilles tendinitis
- Achilles tendon rupture
- Stress fractures
- Tarsal tunnel syndrome
- Plantar fasciitis
Symptoms
Symptoms of ankle injury vary based upon the condition. Pain may include general pain and discomfort, swelling, aching, redness, bruising, burning or stabbing sensations, and/or loss of sensation.
Diagnosis
Due to the wide variety of potential causes of ankle pain, podiatrists will utilize a number of different methods to properly diagnose ankle pain. This can include asking for personal and family medical histories and of any recent injuries. Further diagnosis may include sensation tests, a physical examination, and potentially x-rays or other imaging tests.
Treatment
Just as the range of causes varies widely, so do treatments. Some more common treatments are rest, ice packs, keeping pressure off the foot, orthotics and braces, medication for inflammation and pain, and surgery.
If you have any questions, please feel free to contact our office located in Findlay, OH . We offer the newest diagnostic and treatment technologies for all your foot care needs.
The Power of Running Is Enhanced by Wearing Proper Footwear

Running offers a multitude of benefits for both physical and mental well-being. It strengthens the cardiovascular system, improves lung function, and boosts metabolism, aiding in weight management and overall health. Beyond the physical advantages, running also promotes mental clarity, stress relief, and a sense of accomplishment. However, to reap these benefits safely and effectively, investing in good running shoes is vital. Quality footwear provides essential support, cushioning, and stability, reducing the risk of injuries such as sprains, strains, and stress fractures. Proper running shoes are designed to accommodate the unique biomechanics of each individual, offering optimal shock absorption and alignment for a smoother, more comfortable stride. By selecting the right shoes for their foot type and running style, runners can enhance performance, minimize discomfort, and prolong their running journey, ensuring they can continue to enjoy the myriad benefits that running has to offer for years to come. Injuries to the foot and ankle can happen from running, and it is essential the right running shoes are chosen. It is suggested that you contact a podiatrist who can treat foot and ankle injuries, and guide you on what the best type of running shoes are right for you.
You should always make sure your running shoes fit properly in order to avoid injury. For more information, contact Thomas Vail, DPM from Step Alive Foot & Ankle Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
Choosing the Right Running Shoe for Your Foot Type
Improper shoe sizing can cause a myriad of problems for your feet. Shoes that don’t fit you properly can lead to muscular imbalances in your body, which can result in foot, knee, and hip injuries.
Tips for Finding the Right Running Shoe
- Make sure you have a thumb’s width of wiggle room between the end of your longest toe and the front of the shoe.
- There should be little to no slipping at the heel
- Don’t assume your size in one shoe brand will be your size in another
- Do not lace up your shoes too tightly
- Walk around in the store with your new shoes before you buy them
If you have any questions please feel free to contact our our office located in Findlay, OH . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Choosing the Right Running Shoe
Choosing the right running shoes for you is an important part of running. A good pair of running shoes will make the running experience more enjoyable for you and prevent potential injury.
Poorly-fitted shoes can increase the risk of injury in runners substantially. Common injuries from running with poor quality shoes include shin splints, sprained ankles, Achilles tendinitis, stress fractures, plantar fasciitis and more. This is due to the fact that bad shoes do not provide proper foot support, can increase pronation (how much the foot rolls when hitting the ground), have little to no cushioning, do not allow the feet to breath, and do not provide enough flex and rigidity in the right parts.
When looking for running shoes, first, determine where you will be running. If you are a trail runner, then pick trail shoes. If you run on concrete and asphalt, then regular running shoes are the best choice. When trying on shoes, its best to go at the end of the day as feet grow during the day and shrink after a night of sleep. Shoes should be more rigid towards the back of the foot while being more flexible up where the toes are. The toe box should provide enough room for the toes to move freely. The overall fit should be snug, not too tight but not too loose. A good pair of running shoes should also provide enough arch support for your foot type. If you experience overpronation or under-pronation while running, try to find a pair of shoes that will help correct this with different sole patterns. Finally, try to find a pair of shoes that allow the feet to breathe like nylon mesh or synthetic leather.
Don’t forget about the socks either. Socks that hold too much moisture can lead to athlete’s foot. Socks should be breathable so that your feet can air out and breathe. Synthetic socks wick away moisture like sweat. If you tend to run a lot, having a second pair of shoes that you can wear while you let the first pair air out is smart. Just don’t forget to replace your shoes after about every 300 to 500 miles.
Before you start running, it is advised to see a podiatrist to see if running is right for you. They can also offer good advice on how to run and what to look for in a pair of running shoes. If you have flat feet or poorly supported ones, they can also offer custom-made orthotics that will help give your feet the support they need.
Athlete's Foot
Athlete’s foot is an extremely contagious infection caused by a fungus that results in itching, burning, dry, and flaking feet. The fungus that causes athlete’s foot is known as tinea pedis and thrives in moist, dark areas such as shower floors, gyms, socks and shoes, commons areas, public changing areas, bathrooms, dormitory style houses, locker rooms, and public swimming pools. Athlete’s foot is difficult to treat as well because of the highly contagious and recurrent nature of the fungus.
Tinea is the same fungus that causes ringworm, and is spread by direct contact with an infected body part, contaminated clothing, or by touching other objects and body parts that have been exposed to the fungus. Because the feet are an ideal place for tinea to grow and spread, this is the most commonly affected area. It is, however, known to grow in other places. The term athlete’s foot describes tinea that grows strictly on the feet.
The most commonly infected body parts are the hands, groin, and scalp, as well as the feet. Around 70% of the population suffer from tinea infections at some point in their lives, however not all of these cases are athlete’s foot. Just like any other ailment, some people are more likely to get it than others, such as people with a history of tinea infections or other skin infections, both recurring and non-recurring ones. The extent to which a person experiences regrowth and recurrent tinea infections varies from person to person.
Sometimes people will not even know that they are infected with tinea or that they have athlete’s foot because of a lack of symptoms. However, most experience mild to moderate flaking, itching, redness, and burning. However, some of the more severe symptoms include cracking and bleeding skin, intense itching and burning, pain while walking or standing, and even blistering.
Because of the recurring nature of the tinea fungus and the athlete’s foot it causes, the best way to treat this condition is with prevention. You can take some preventative measures such as wearing flip flops or sandals in locker rooms and public showers to reduce contact with the floor. It also helps to keep clean, dry feet while allowing them to breathe. Using powders to keep your feet dry is a good idea, as well as keeping your feet exposed to light and cool air, to prevent the growth of tinea. If you do happen to get athlete’s foot, opt for using topical medicated creams, ointments or sprays. These treatments help eliminate and prevent it from coming back.
What Is Toenail Fungus and How Is It Treated?

Toenail fungus, medically termed onychomycosis, is a fungal infection that commonly affects the toenails. It is typically caused by dermatophytes, which are fungi that thrive in warm and moist environments like sweaty shoes or public swimming pools. When these fungi invade the toenail bed, they can cause discoloration, thickening, and crumbling of the nail. Symptoms may include yellowing or darkening of the nail, a distorted shape, and a foul odor. Certain factors increase the risk of developing toenail fungus. Among them are age, poor circulation, weakened immune system, and frequent exposure to moist environments. Common types of fungal infections include distal subungual onychomycosis, white superficial onychomycosis, proximal subungual onychomycosis, and candida onychomycosis. Treatment typically involves prescribed antifungal medications, either topical or oral, depending on the severity of the infection. In severe cases, surgical removal of the nail may be necessary. If you think you have toenail fungus, it is suggested that you schedule an appointment with a podiatrist for a proper diagnosis and treatment at your earliest convenience.
Athlete’s foot is an inconvenient condition that can be easily reduced with the proper treatment. If you have any concerns about your feet and ankles, contact Thomas Vail, DPM from Step Alive Foot & Ankle Center. Our doctor will treat your foot and ankle needs.
Athlete’s Foot: The Sole Story
Athlete's foot, also known as tinea pedis, can be an extremely contagious foot infection. It is commonly contracted in public changing areas and bathrooms, dormitory style living quarters, around locker rooms and public swimming pools, or anywhere your feet often come into contact with other people.
Solutions to Combat Athlete’s Foot
- Hydrate your feet by using lotion
- Exfoliate
- Buff off nails
- Use of anti-fungal products
- Examine your feet and visit your doctor if any suspicious blisters or cuts develop
Athlete’s foot can cause many irritating symptoms such as dry and flaking skin, itching, and redness. Some more severe symptoms can include bleeding and cracked skin, intense itching and burning, and even pain when walking. In the worst cases, Athlete’s foot can cause blistering as well. Speak to your podiatrist for a better understanding of the different causes of Athlete’s foot, as well as help in determining which treatment options are best for you.
If you have any questions please feel free to contact our office located in Findlay, OH . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
See Your Foot Specialist Regularly If You Work On Your Feet
Wound Care
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
Causes and Definition of Foot Ulcers
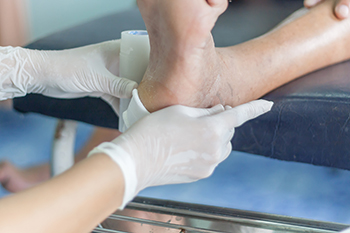
Foot ulcers are open wounds that develop on the feet, often affecting individuals with diabetes or impaired circulation. They typically occur due to a combination of factors, including neuropathy, which is nerve damage, poor blood flow, and pressure from footwear. Foot ulcers can vary in severity, from shallow sores to deep craters, and if left untreated, they can lead to serious complications such as infection and possibly amputation. The primary cause of foot ulcers is prolonged pressure or friction on the skin, which can result from wearing ill-fitting shoes, walking barefoot, or excessive rubbing. In diabetic individuals, high blood sugar levels can further exacerbate the risk by damaging nerves and blood vessels, impairing the body's ability to heal. Other contributing factors may include poor hygiene, smoking, obesity, and a history of foot problems. Recognizing the signs of a foot ulcer, such as redness, swelling, or drainage, is vital for prompt treatment and prevention of complications. If you have a foot wound, it is strongly suggested that you consult a podiatrist who can diagnose its severity, and offer treatment options that are right for you.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with Thomas Vail, DPM from Step Alive Foot & Ankle Center. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our office located in Findlay, OH . We offer the newest diagnostic and treatment technologies for all your foot care needs.

